|
By Alexandra Bunjes The global contraceptives industry earns approximately $20 billion per year and is expected to increase to $33 billion by 2023 [7]. The majority of this money goes towards female-targeted methods of pregnancy prevention such as oral contraceptives, intrauterine devices (IUDs), condoms, implants, and injectables. Ninety-eight percent of women in the United States have used contraception at some point in their lives and 62% of women in the US of reproductive age are currently using birth control methods [4]. Due in part to the efficacy of female contraception and its widespread nature, women carry much of the responsibility for pregnancy prevention and there isn’t much research incentive to explore methods that are targeted to men.
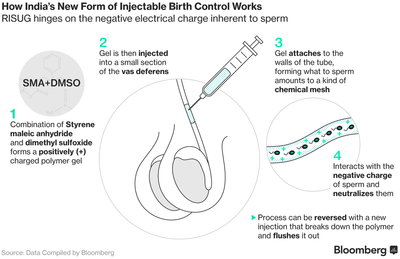
Currently there are no prescribed hormonal methods of birth control for men, but why? It may seem to be a normative standard that women bear the brunt of the responsibility for pregnancy prevention, but why is this? Why does female-geared contraception dominate the market? Why isn’t male birth control as prevalent as female birth control? The answers to these questions ultimately boil down to two problems: the biological difficulty of creating male birth control and the lack of incentive of pharmaceutical companies to sell it. Contraception was initially created for women because they were typically the ones who bore the responsibility for childrearing. However, research has since indicated another reason why today more contraception is still targeted toward women: female reproductive biology leaves more room for interference. Since women have a regulated monthly cycle, small doses of hormones each day – through oral contraception, arm implants, or injections – can be very effective in altering the process to decrease chances of pregnancy. Additionally, IUDs can either release hormones or be made of materials that divert sperm. IUDs are placed in in the uterus, so even if pregnancies do implant, it is difficult for them to progress. Male biology is much different: each month, a female only produces one mature egg, but men produce millions of sperm. Since women cyclically release one product, it is easier to influence this process than continual male spermatogenesis [8]. Hormonal pills would also take weeks to affect sperm count [8] and previous clinical studies have shown that in order to have contraception in men of comparable efficacy to that in women, large amounts of hormone must be administered, which often causes long-term adverse effects [2]. Many male hormonal studies up until this point have caused acne and mood disorders, which has discouraged participants from wanting to continue. There is also no simple way to directly interfere with the male reproductive organs in a manner similar to that with an IUD. Nonetheless, many researchers have remained committed to exploring the potential for male contraceptives with the hope of shifting some of the responsibility. In 2016, an experiment was done in which healthy men between the ages of 18 and 45 were injected with hormonal birth control every eight weeks [2]. Couples participating in this study were in monogamous and had an average coital frequency of twice per week [2]. The hormone injection involved a mix of the sex hormones progestogen and testosterone. This caused suppression of sperm production and a decreased number of pregnancies. By 24 weeks into the experiment – after 3 rounds of injections – participants showed a significant decrease in sperm concentration [2]. Additionally, there was a 95% rate of recovery after 54 weeks, which means that sperm production returned to normal. Of the 266 male participants in this experiment, four of their partners became pregnant, yielding an overall failure rate of 1.57% [2]. Side effects included acne, mood changes, increased libido, and injection site pain – circumstances not dissimilar to what women experience each month on their periods or while taking oral birth control [2]. This experiment was terminated early due to the frequency of mood disorders, but it nonetheless demonstrated the potential for hormonal male birth control to become a viable method of contraception. Arguably, the most promising method is the gel injections developed by 76-year-old biomedical engineer Sujoy Guha. These injections are quick, reversible, and have demonstrated 98% effectiveness in preventing pregnancy with no major side effects [1]. The procedure is simple: the sperm-carrying tubes in the scrotum are injected with a polymer gel that damages the heads and tails of the sperm, effectively disabling them and thus preventing them from being able to swim to the egg and fertilize it. This gel was injected into 540 men in India 13 years ago, and none have had pregnancies since their injection. This contraceptive effect lasts until reversed by a second injection, which breaks down the gel and allows normal reproduction to continue. The U.S. nonprofit Parsemus Foundation is working to establish a market for the gel outside of India with the goal of selling the injections for as low as $10 in poorer countries and for a few hundred in richer ones [1]. The foundation is currently raising funds to conduct human trials [1]. Since this gel is cheap, unlike IUDs, and does not require constant administration, such as birth control, it could be revolutionary for the 225 million women in developing countries that do not have access to contraception [1]. Worldwide projections estimate that putting this gel on the market would result in a $10 billion drop in the female contraception market and $3.2 billion overtaking of annual condom sales. The current issue that Guha faces with his injections is finding a company to sell them – Big Pharma is not interested in male contraception [1]. This is an example of the social problems that underlie male contraceptive development: the success of female contraception and the frustrating prevalence of reproductive inequality has caused there to be little incentive for male birth control to be developed and marketed. The prevalence of female birth control has normalized female responsibility, and despite the research being done surrounding male contraception, most men are wary of taking control of pregnancy prevention. Since the market for female contraception shows no signs of diminishing and most of the leaders in pharmaceutical companies are men, male birth control has been given little attention. Nonetheless, the results of these the gel and hormone therapy studies indicate that progress is being made toward a more equal balance of reproductive responsibility. Since there are many steps to be taken between creation and implementation, the success of this research does not mean that other studies have stopped; researchers are continuing to find new ways to address the topic of male reproduction. Some studies are taking a closer look at sperm production and trying to stop it at its source. When sperm are released during ejaculation, they use a corkscrew-like motion to drill into the egg and inject genetic material [6]. This is made possible by an ion channel called Catsper, which is only found in sperm [6]. One potential method of future birth control could be looking for ways to block up this channel and thereby prevent sperm from drilling into eggs. Another way of exploring this issue is by learning about the mechanisms underlying male infertility and then finding ways to apply this knowledge for contraceptive use. For example, about 10% of infertile men have disruption in the fertility-causing genes of their Y chromosomes [5]. Since it is known that deletion in any of three specific regions leads to infertility, exploring the roles of these genes could lead us to back-solving for contraception; if we know exactly what the genes do – and thus why their absence is leading to infertility – we could potentially develop targeted drugs that inhibit the sperm, thus blocking pregnancy [5]. This ties into another concept being explored in male birth control: the notion of turning the “switch” of contraception on and off. The ideal circumstance for birth control would be to find a reliable, reversible way to turn off sperm production or prevent sperm activity. One proposed method for doing this is to try to block the gene that prevents sperm from being damaged during production. In a study with mice, it was shown that the lack of this protective gene can lead to infertility because sperm production comes to a halt [5]. If scientists could find ways to control this, it is another potential avenue for pregnancy prevention [5]. There are clearly many exciting areas of research being explored when it comes to male contraception, but there aren’t many pharmaceutical companies willing to invest in distribution. The hope is that in the coming years, demand will increase, and the responsibility for contraception will shift from women to become more of a shared undertaking. This would be a big step toward not only reducing the instances of unplanned pregnancy, but also reaching a state of increased reproductive equality. References 1. Altstedter, A. (2017, March). A New Kind of Male Birth Control Is Coming: Novel treatment may be submitted for Indian approval this year. Bloomberg. Retrieved from https://www.bloomberg.com/ 2. Behre, H. M., Zitzmann, M., Anderson, R. A., Handelsman, D. J., Lestari, S. W., McLachlan, R. I., ... & Festin, M. P. R. (2016). Efficacy and safety of an injectable combination hormonal contraceptive for men. The Journal of Clinical Endocrinology & Metabolism, 101(12), 4779-4788. 3. Jegalian, Karin & Lahn, Bruce. (2001). Why the Y is so Weird. Scientific American - SCI AMER. 284. 56-61. 10.1038/scientificamerican0201-56. 4. Jones, J., Mosher, W., & Daniels, K. (2013). Current contraceptive use in the united states, 2006-2010, and changes in patterns of use since 1995. In Sexual Statistics: Select Reports from the National Center for Health Statistics. Nova Science Publishers, Inc.. 5. Michigan State University. (2017, October 10). Genetic advance for male birth control.ScienceDaily. Retrieved October 16, 2017 from www.sciencedaily.com/releases/2017/10/171010124108.htm 6. Molteni, Megan (2017, May). Scientists Found Sperm’s Power Switch – And a Way to Turn It Off. Wired Magazine. Retrieved from https://www.wired.com/ 7. Nasdaq GlobeNewswire (2016, September 27). Contraceptives Market size to exceed $33 Billion by 2023: Global Market Insights Inc. Retrieved from https://globenewswire.com/ 8. Smith, B. C. (2017, August). Here’s Where We’re at With the ‘Male Pill’ – ‘We’ve been 5 years from male contraception for 50 years.’ Mel Magazine. Retrieved from https://melmagazine.com
2 Comments
Patricia Barnes
11/22/2022 06:58:25 am
Kamagra Polo https://www.pharmaglobalrx.com/kamagra-polo.html which inhibits the activity of cGMP-specific phosphodiesterase type-5 (PDE-5) and treats erectile dysfunction. This enzyme degrades the neurotransmitter cGMP, which causes smooth muscles to relax.
Reply
Leave a Reply. |
Executive Board 2017-2018
President/Editor-In-Chief- Jane Donnelly ('19) Assistant Editor in Chief- Anna Molotkova ('20) Treasurer- Amy Meng ('19) Layout Editor- Clare Foley ('19) Events Coordinator- Tim Ring ('20) Categories |

 RSS Feed
RSS Feed
